Patients suffering from esophageal cancer may someday get transplants fashioned from their own stem cells, thanks in part to new controller technology that lets researchers grow new human organs.
The technology comes from a company called Biostage Inc. The firm has come up with a way to take mesenchymal stem cells from a cancer patient and seed them on a biocompatible scaffold. After about seven weeks in a bioreactor, the scaffold seeded with the patient’s own cells gets implanted in the patient to replace the diseased esophagus. Eventually, the scaffold is removed using minimally invasive surgery, leaving a functioning and disease-free esophagus.
 Right now, the only patients who have received Biostage’s regrown esoaphagus transplants are some 30 pigs, says Biostage chief medical officer and executive vice president Saverio LaFrancesca. The company hopes to run a human clinical trial sometime in 2017.
Right now, the only patients who have received Biostage’s regrown esoaphagus transplants are some 30 pigs, says Biostage chief medical officer and executive vice president Saverio LaFrancesca. The company hopes to run a human clinical trial sometime in 2017.

A Biostage bioreactor chamber, outfitted for demonstration purposes with colored water and a cylindrical plastic form. The cylindrical form continuously rotates in the water. If this were in a real setting, a cylindrical scaffold would take the place of the plastic form. It would rotate in a bath of cells expanded from a few biopsied from the patient.
Biostage’s technology, which it calls Cellframe, employs a multistep process in which the patient’s own stem cells are taken from a simple adipose/fat tissue biopsy, then get expanded and banked. They are then seeded onto the proprietary scaffold that mimics the natural dimensions of the organ being regenerated. In the case of an esophagus, the scaffold basically has a cylindrical shape. After several days in a rotating bioreactor, the stem-cell-containing scaffold is ready to be implanted. Biostage says its Cellframe technology is designed to deliver the necessary cues for triggering, guiding and modulating the regenerative process.
In May, Biostage announced positive proof-of-concept results in large-animal studies for the esophageal implant conducted with the Mayo Clinic. It is also preparing an article about the technique for a peer-reviewed scientific journal. It says the next step is to execute these same studies under Good Laboratory Practice (GLP) standards — GLP refers to a quality system to ensure safety and reproducibility according to FDA standards and is a key milestone on the way to initiating trials in humans.
Biostage also expects to follow the esophageal implants with additional products to address life-threatening conditions of the bronchus and trachea.

Jeff Bouchard and a Biostage Cellframe clinical controller.
The bioreactors are run from a controller that is basically a Single-Board RIO controller (sbRIO-9627) from National Instruments. According to Biostage control systems manager Jeffrey Bouchard, the Biostage controller requires many system-level functions such as FTP, SQL, email, and remote access, which were developed using the NI LabVIEW program. Biostage uses the FPGAs on the RIO controller to add redundant and time-sensitive controls. Once The FPGA manages the direct interaction with the bioreactor independently and also provides life support by monitoring the real-time application. It can also reboot in case of a rare failure, Bouchard says.
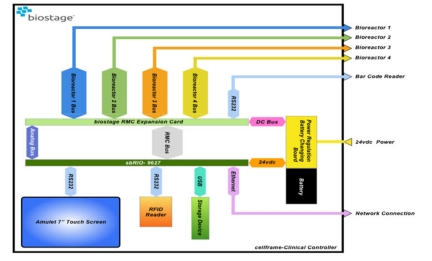
Biostage Controller Block Diagram
One RIO-based controller can support four bioreactors, Bouchard says. The bioreactor bus is a proprietary network that supports many forms of regenerative medicine bioreactors. The controller manages the rotation and position of an organ implant while also handling the perfusion process (pressure, media types, temperature, pH, and so forth). The controller as well monitors environmental conditions such as temperature, humidity, gas levels, and the condition of cell culture media during the incubation phase. And it takes care of imaging that shows the progress of organ development.
The post Clever instrumentation plays a role in
growing new human organs appeared first on Test & Measurement Tips.