Engineers who usually spend a significant amount of their time around test instruments are likely spending more of it at home these days. Those of us who’s working life has been interrupted by the Covid-19 virus might well begin pondering about what goes into a test for human viruses rather than those confined to computers. Here’s a quick review of what happens once a nurse takes a mouth swab.
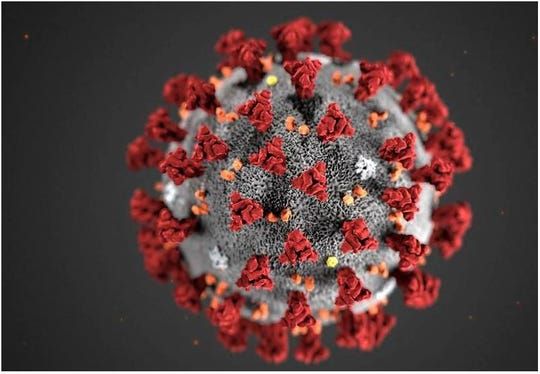
The Covid-19 virus particle as depicted by the Centers for Disease Control and Prevention.
In general, lab tests for viruses fall into two categories: Molecular or genetic tests, which look for evidence of active infection; and serology tests, which look for a previous infection by detecting antibodies. The Covid-19 tests being run in the U.S. as of this writing are strictly molecular tests. They were made possible on Jan. 12 after Chinese scientists published the virus’s genomic sequence.
In a nutshell, genetic tests look for the genes of the virus. The molecular tests now underway are generally real-time reverse-transcription polymerase chain reaction (rRT-PCR) assays. Viruses store their genetic code in RNA, rather than DNA. Thus the first step in the test is to copy any collected RNA into DNA using an enzyme called reverse transcriptase. The DNA is then amplified into billions of copies, called amplicons, via the polymerase chain reaction (PCR) process. The resulting sample is sequenced and compared with the sequence expected if the starting point was virus RNA.
There are various ways to monitor the amplification of targeted DNA during the PCR reaction. One method, called rRT-PCR, monitors the amplification progress using fluorescent technology. As the number of DNA amplification copies rises during the PCR reaction, so too does the fluorescence. The fluorescence serves as a way of monitoring the PCR reaction in real time.
To the layman, this sort of genetic testing may sound complicated, but the equipment necessary to run it is commonplace in hospitals. The method begins with the placement of one or two sample test tubes in an apparatus called a thermal cycler. The cycler raises and lowers the temperature of a thermal block holding the test tubes in discrete, pre-programmed steps. All the steps through amplification take place in the thermal cycler.
To actually separate out the DNA of interest, a technique called gel electrophoresis might be used. Here an electric field pushes the molecules to be separated through a gel containing small pores. The molecules travel through the pores in the gel at a speed that is inversely related to their lengths. Thus a small DNA molecule travels a greater distance through the gel than will a larger DNA molecule.
It takes a while to run through all these steps. Currently, authorities are quoting turn-around times of a day or more for test results. But there are new techniques in the wings that are said to provide results in a couple of hours.
Presently there is also great interest in developing serology tests for Covid-19. That’s because it’s important to know who has been infected in the past and recovered as a basis for understanding how the virus spreads through a population.
A serology test is basically a blood test. It uses a protein, called an antigen, to harvest antibodies from a blood sample. Most tests under development focus on a spike-shaped protein that sticks out in many places from the surface of the virus particle.
A typical serology test would involve nothing more than a special reagent. A blood sample would go into a test tube coated inside with a reagent whose molecules bind specifically to Covid-19 antibodies. A positive result could produce a color change or perhaps fluorescence to indicate success. In tests under investigation so far, the whole test finishes in about 15 minutes.