It is now trivial and non-invasive to measure blood-oxygen saturation SpO2, thanks to LEDs, algorithms, and ICs for pulse oximetry — it’s a very long way from having to draw blood and send it out for assessment.
Part 1 of this FAQ discussed the principle of the non-invasive, light-based pulse-oximetry systems for reading blood-oxygen saturation SpO2, and some of the issues that such a system must overcome. Part 2 will show how ICs and associated components provide a high-performance, nearly complete pulse-oximetry system at low cost and low power.
Q: What are some of the other issues that a design must overcome?
A: There are many:
- Ambient light: even if the arrangement is optically shielded, stray light from nearby and overhead lights will reach the photosensor, largely due to the internal-scattering effect. In addition, the ambient light “noise” light varies significantly as the patient or nearby people move, and block/unblock overhead or outside light. The system must dynamically adjust to these changes and even use adaptive, hardware-based gain-ranging to provide the needed dynamic range and avoid saturation of the photodetector.
- Temperature coefficients: For both LEDs, their output intensity and wavelength affected by temperature; the response curve of the photosensor is also temperature sensitive. The algorithm must factor these shifts into its processing via real-time corrections.
- LED drive current and pulse width: there is an optimum LED drive and output level which maximizes their dynamic range and performance. These parameters are functions of the individual LEDs used, will vary from batch to batch, and even change as the LED ages. The system must continuously adjust the current for each LED to maintain it at the optimum drive value. The visible and IR LEDs are pulsed alternately, and the specific pulse widths are a tradeoff between performance (longer pulse widths provide better results) versus power-consumption and self-hearting concerns. Typical pulse repetition frequency is 100 Hz with a duty cycle of 25%.
- Sampling rate: as with most biological processes, things are relatively “slow” so the SpO2-related sampling rates are between about 100 samples/sec (sps) and a few ksps. On the other hand, the required resolution is on the higher side, with 16 bits as a minimum but with most systems using between 18 and 22 bits. The ADC front-end subsystem must be programmable over a wide range to accommodate different LED/photosensor pairings, patient skin type, tissue density, and digit thickness, each of which will affect the minimum/maximum values of the electrical-optical-electrical path.
References 2 through 5 give insight into the enormous amount of research and validation needed to go from the basic concept to an accurate system which correlates light transmission and wavelengths with actual SpO2 numbers. Despite these challenges, the industry has succeeded so well that you can buy a clip-on meter at any pharmacy or Walmart, or similar mass-market outlets, Figure 1.
Fig 1: Using modern, low-power, high-performance optical, analog, and digital components, a fully integrated SpO2 sensing system and readout can fit on a fingertip clip and retail for very modest price. Source: YouTube
Q: How are ICs used to build an SpO2 system?
A: The IC provides two functional blocks: an analog front end (AFE) for the LED drive and photosensor output including digitization, and a processing function for the critical algorithms. The current and pulse width of the LED drivers must be fully controllable, based on guidance from the processed signals. The photosensor needs a transimpedance amplifier (TIA) and amplifier/filter stage to convert the weak photodiode current to a useful voltage, and needs a wide dynamic range (80 to 100 dB).
Q: Who provides these ICs?
A: Given the huge market opportunity for both clinical and personal units, as well as the good fit with the analog-centric process technologies which are needed, pulse oximetry is attractive to major IC vendors. Among the sources for standard chipsets and supporting algorithms are Analog Devices, Texas Instruments, Maxim Integrated, Silicon Labs, and Microchip Technology. There are also vendors of custom ASICs, but these are not standard open-market components.
Q: What does a typical IC or chipset look like?
A: The MAX30102 from Maxim Integrated is an integrated pulse-oximetry and heart-rate monitor non-monolithic module which includes internal LEDs, photodetector, optical elements, and low-noise AFE electronics, Figure 2, plus a temperature sensor and other peripheral functions. The fully conditioned, calibrated, and digitized optical-output data provided by the MAX30102 goes via an I2C port to a user-selected system microcontroller which implements the SpO2 algorithms.
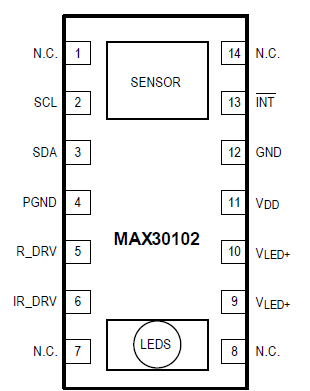
Fig 2: The MAX30102 is a multichip IC which includes all the AFE functions, and communicates with its processor via an I2C port (not shown are some internal AFE blocks such as TIA, gain amplifiers, and analog filters). (Source: Maxim Integrated)
Q: What about packaging?
A: Unlike “conventional” ICs and electronics, the packaging of this device is unusual: it is a 14-pin optical module with integrated cover glass (just 5.6 × 3.3 × 1.55 mm), Figure 3, to be mounted within the finger clip. Power requirements are very low, at under 1 mW in active mode and 0.7 μA in shutdown from a 1.8 V and a separately boosted 5.0-V rail for the LEDs. Using this arrangement, the battery, power converters, MAX30102, microcontroller, and readout can fit into a single clip-on housing.
Fig 3: Unlike most ICs, the physical layout of the MAX30102 subsections is an inherent part of its application, putting the LEDs on one side and the sensor on the other; the patient’s finger is to be interposed between source and sensor sides. (Source: Maxim Integrated)
Q: Where do the algorithms come from?
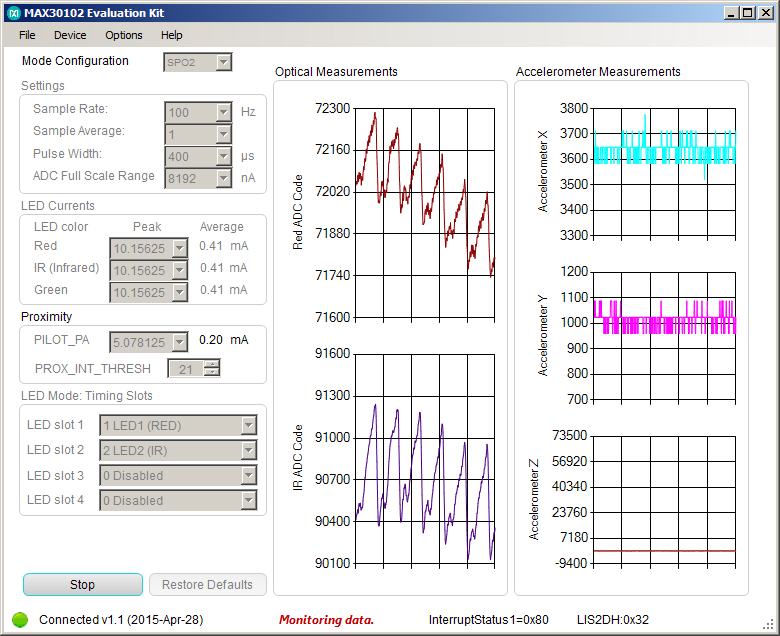
A: Vendors such as Maxim provide basic code blocks, but each OEM must develop (and get approval) for their enhancements the device is to be used for more than casual situations. A development system/evaluation module from Maxim offers two different medical-standard algorithms which designers can use as starting points (not shippable code) for developing and enhancing their own final code used to calculate SpO2 and heart rate. Access and evaluation is via a graphical user interface (GUI) supplied with the development system, Figure 4.
Fig 4: Through the GUI of the evaluation kit, users can vary LED drive parameters such as current and see the effects on photosensor output; they can also adjust ADC sampling rate and other AFE operating condition. (Source: Maxim Integrated)
Q: What are the functions of the basic algorithms they offer for evaluation?
A: The PBA algorithm looks for zero crossings using a slow threshold and completes its evaluation cycle with each sampling point, so it has no output delay. In contrast, the SKA algorithm waits for three seconds and then looks for a peak; it cycles at a higher rate of once per second but it requires a more-complex math operation. Also, PBA requires much less data space and code space compared to SKA.
Q: What type of circuit enhancement might be added by an OEM?
A: Some OEMs add a MEMS-based three-axis accelerometer for wearable applications, to compensate for user motion while making measurements.
Q: Finally, a question that every engineer must ask: what about test and validation?
A: It’s a split answer, with one part being fairly straightforward, but the other part being fairly difficult.
Q: How so?
A: The circuitry signal chain can be evaluated by driving the LEDs over a wide range of currents and conditions, then adding optical noise (different amounts of ambient light along with minute physical motion) as well as EMI/RFI corruption to the electrical signals.
However, there are no simulators which can replicate the patient’s finger and blood with different SpO2 levels; Reference 6 is an insightful discussion of the situation and evaluation options. Therefore, the design team must have a plan for verification which uses methods and techniques which have been established by the medical community and regulatory agencies.
This FAQ has looked at how modern electronic and electro-optical components (LEDs, photosensors, ICs) and algorithms executing in microcontrollers have changed measurement of blood-oxygen level from an unpleasant, risky, intrusive blood draw to a simple, real-time, finger-clip function. It is a good example of how this combination is dramatically changing the world of medical instrumentation, as well as moving it from the clinic to the home and person.
References
- org, “History of Pulse Oximetry.”
- American Thoracic Society, “Pulse oximetry”
- Ashfaq Hasan, Handbook of Blood Gas/Acid-Base Interpretation, Chapter 2: “The Non-Invasive Monitoring of Blood Oxygen and Carbon Dioxide Levels,” (Springer).
- “Independent Component Analysis Applied to Pulse Oximetry in the Estimation of the Arterial Oxygen Saturation (SpO2) – a Comparative Study” (Annual Conference of the IEEE Engineering in Medicine and Biology Society, 2009)
- Texas Instruments, SLAA655, “How to Design Peripheral Oxygen Saturation (SpO2) and Optical Heart Rate Monitoring (OHRM) Systems Using the AFE4403”
- Fluke Biomedical, “There’s no such thing as a SpO2 simulator.”
Resources
NCOA, “How to Use a Pulse Oximeter”






Do you have a technological background to determine blood glucose in diabetic people, using sensors similar to pulse oximetry? Thank you
No, but I have read about work being done. It’s a difficult technical challenge plus the verification and approval process is very long.